Root Resorption comes in 2 flavors, so to speak: Internal and External. It’s one of the least common reasons for losing a tooth, compared to tooth decay and gum disease. When it is found though, it usually means the tooth is doomed. But what is root resorption?
Internal & External Root Resorption FAQs
The term “resorption” comes from the Latin root resorbere, meaning “to absorb.” In teeth however, it’s not really absorption like a sponge absorbing water. A tooth being resorbed is actually eaten away, either by cells inside the pulp or outside the root. Because the growing cells shouldn’t be, resorption is a little like cancer. Only a little bit though. That’s because root resorption never spreads, not even to the tooth next to it.
Internal Root Resorption is caused by Pulp Cells
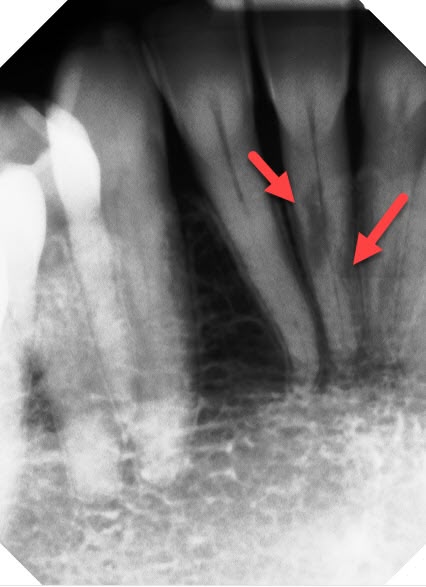
Pulp cells are found in the nerve chamber and canals inside the tooth. They start growing outward, turning the dentin into a sponge-like, soft, mushy mess. It’s usually a very slow process, and it’s rarely painful until it has progressed a lot. Because it usually happens in tooth roots, it’s often not visible on normal x-rays. That means dentists can’t see it, unless there’s a reason to take an x-ray of the whole tooth, as seen here. This was taken in July 2019, on a new patient in our practice. It became sensitive just recently.
Based on this x-ray alone, I didn’t know if this was internal or external resorption. So we took a 3D Cone Beam x-ray, to see it from multiple angles, as seen below. From that, it appears to be internal root resorption. It got big enough to break through the root, which allows bacteria in. That’s probably why it became sensitive recently.
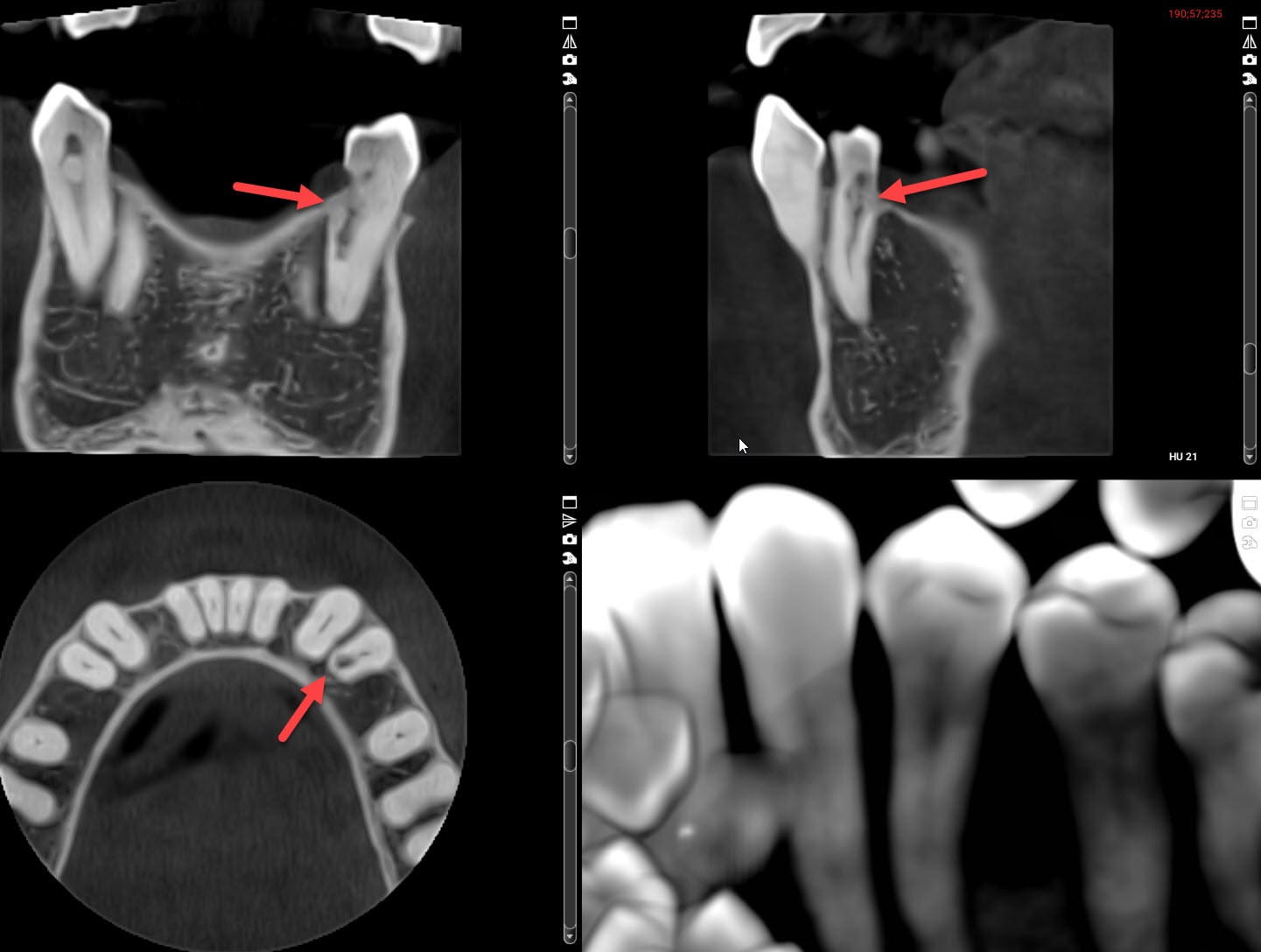
We don’t know yet if this tooth can be saved, but I’ve referred her to a root canal specialist (endodontist) and gum specialist (periodontist). If they can’t save it, we will probably do a dental bridge to replace the tooth. The other tooth roots are too close together for a dental implant. I’ll try to remember to update the post once she makes a decision.
External Root Resorption is caused by Periodontal Ligament Cells
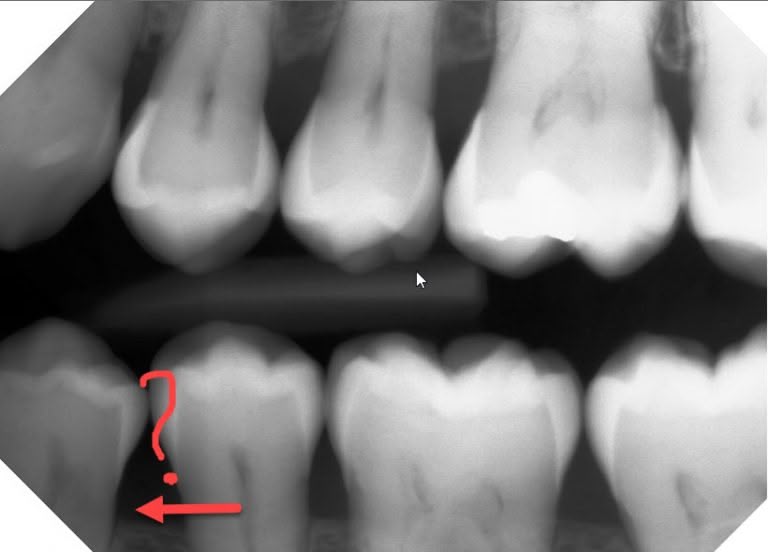
As I mentioned, root resorption is pretty uncommon. In my 20+ years of practicing dentistry, I’ve only come across a few cases. That’s why the patient in the first case above was so unusual. When evaluating the lower front tooth resorption, I noticed a second tooth with resorption, but this time it clearly started outside of the tooth. 2 teeth with resorption on the same patient is odd enough. One tooth with internal resorption and one tooth with external resorption on the same patient??? I’ve never seen, nor even heard of that happening.
It’s a good thing we took the 3D Cone Beam x-ray on the patient though, because we couldn’t see it on the regular bite-wing x-ray at all. This tooth didn’t bother her at all, so we had no reason to suspect it.

Unfortunately, this tooth is definitely not fixable, so it will be extracted and probably replaced with a dental implant and crown. Since it isn’t bothering her and isn’t visible in her smile, we’ll wait until the other tooth is finished.
Inflammatory Root Resorption after Braces
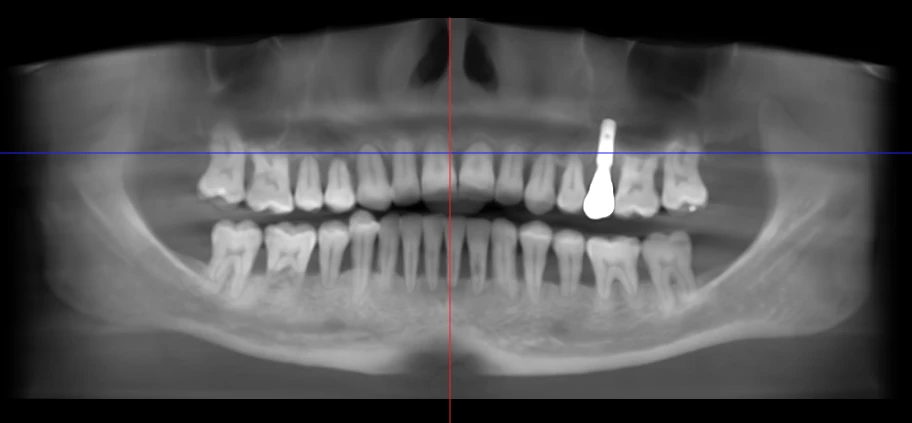
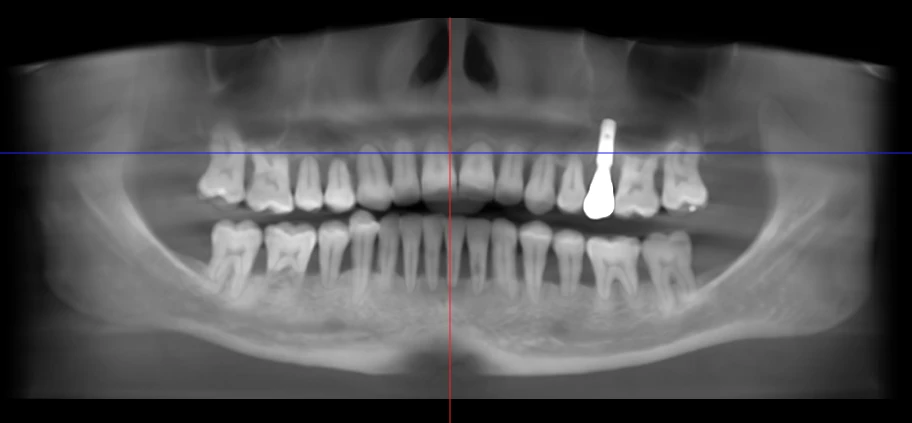
There is one type of root resorption that is unfortunately a bit more uncommon. This kind occurs after aggressive tooth movement, and it seems to have a partially genetic basis. This panoramic x-ray is from a long-time patient in our practice. Her roots have gotten progressively shorter over the years, and now they’re starting to get loose. It’s tragic, but she will probably lose all her teeth within the next couple years. That’s why we’re discussing implant-supported bridges to replace all her teeth soon.
Call us 704-364-7069 or Contact us for a Comprehensive or Emergency Exam.
It’s that easy to start.